At $120 billion per year, chronic kidney disease is responsible for a quarter of Medicare spending—and untold suffering. Early detection with at-home urinalysis can catch the disease early, allow for more effective treatment, and dramatically cut costs for value-based health plans.
Value-based healthcare aims to do small things early and regularly, rather than big things when it’s too late. Linking payments to quality of care gives a better return on investment, reduces systemic waste and—most importantly—improves patient outcomes. But with the shift to value-based care well under way, untapped stores of value are often hard to come by. Chronic kidney disease, or CKD, is the low-hanging fruit hiding in plain sight.
CKD costs $120 billion annually, amounting to nearly a quarter of annual Medicare spending. Due to its progressive nature, the cost of CKD treatment increases exponentially over time. The later stages of the disease are accompanied by very high treatment and hospitalization costs, accounting for a disproportionate amount of CKD expenditures. Hemodialysis, which costs $90,000 per patient annually, is exactly the sort of expensive, late-stage care incentivized by fee-for-service models. A value-based approach offers better solutions.
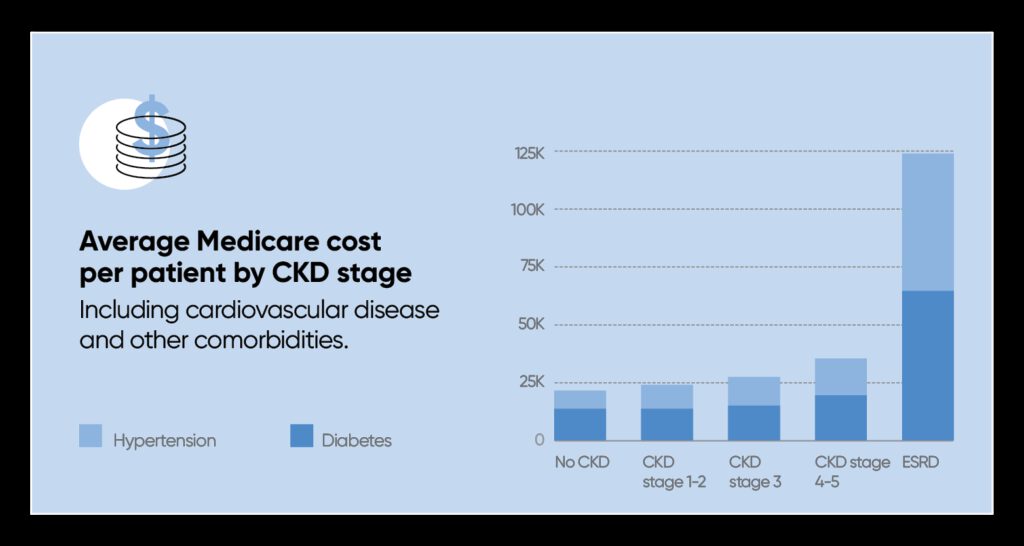
Unlocking Value with Early Detection
Healthy.io’s Minuteful Kidney allows healthcare plans to test the large untested populations of people at-risk for CKD, identifying cases that would have otherwise gone undetected during the asymptomatic early stages of the disease. The test measures the ratio of albumin to creatinine (ACR) in urine, which provides an actionable early indicator of the disease. Both the American Diabetes Association and the National Kidney Foundation recommend annual ACR testing for those at risk for CKD, reflecting a broad consensus of its importance. But testing rates for at-risk people—those with diabetes or hypertension—are as low as 20% on weighted average.
Minteful Kidney has been shown to substantially improve testing adherence, by shifting testing from the clinic to people’s homes, allowing them to test safely and comfortably using a test kit and their smartphone. Now, payers can invest early in an inexpensive urine test rather than hospital fees, dialysis and surgery further down the line.
We commissioned an external actuarial evaluation to find out exactly how payers can benefit from our early detection service. The robust model is based on medical and pharmacy claims data by Optum representing 4.9 million members managed under Medicare Advantage and 12.7 million members managed under commercial plans. The model shows that early detection of CKD with at-home testing delivers powerful outcomes to health plans.
Early Interventions to Reduce Cost of Care
In the early stages of CKD, meaningful medical and lifestyle interventions, such as controlling blood pressure and managing diabetes, can be made to slow the progress of the disease. Additionally, the results of new clinical trials suggest promising outcomes for the use of sodium-glucose cotransporter 2 inhibitors (SGLT-2), particularly when administered to patients in the early stages of CKD.
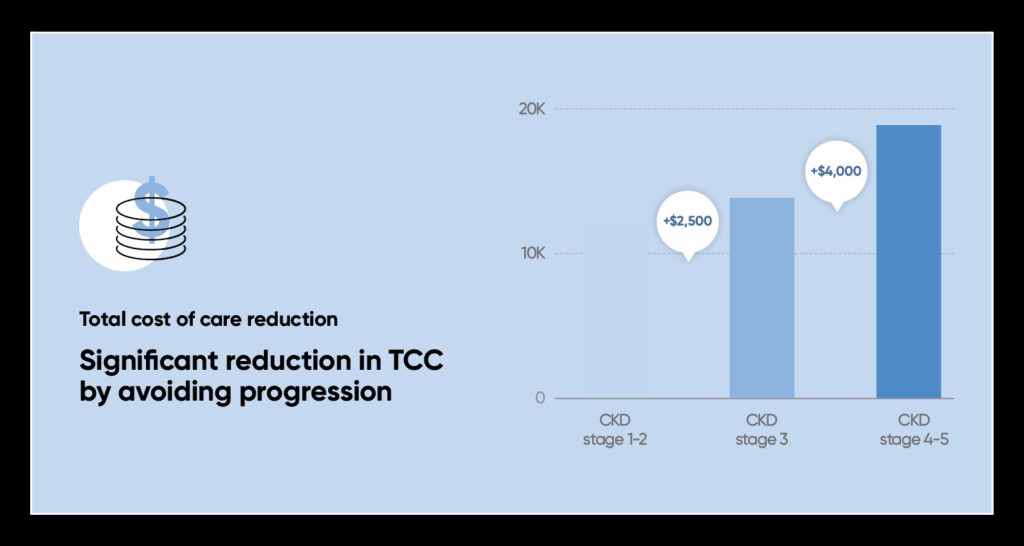
But since CKD is asymptomatic in its early stages, it often goes undetected until its later stages, when the cost of treatment rises dramatically. Raising adherence to early testing translates into more early-stage interventions that reduce disease progression, hospitalization and associated cardiovascular events. The reduction in hospitalization is of special importance, because readmission rates and longer length of stay account for almost 80% of the cost increase with CKD progression. Such early interventions result in a significant reduction in the total cost of care.
Better Risk Scoring
Detecting CKD early also allows for more accurate risk scoring. The evaluation found that due to low ACR testing rates, a significant number of members with diabetes received inaccurate HCC codes—the codes that estimate each member’s risk and anticipated future healthcare costs. Those patients were classified as having no complication, leading to miscalculations of the risk and severity of their condition. An ACR test would correctly identify them as having CKD, leading to a correct risk score, providing for better financial planning for such members’ future course of care, and contributing directly to the ROI.
Net Gains and ROI
The evaluation demonstrated that using Minuteful Kidney Service yields a net gain of $665 per identified Medicare Advantage member over two years and a positive ROI per member within two years, due to the reduction in total cost of care and improved risk scoring. Net gain is calculated assuming proper management and treatment of the disease after diagnosis.
Boosting Quality Metrics
Identifying undiagnosed cases of CKD can also help health plans improve quality performance metrics and make additional gains not calculated in this evaluation. Changes to quality metrics are about to draw more attention to how people experience their care. CMS is substantially increasing the weight of patient experience measures in its Star Ratings, with patient experience anticipated to account for almost a third of plans’ overall Star Ratings by 2023.
Chronic kidney disease is expected to remain a significant and growing burden in the years to come. The abysmally low awareness of the disease means that healthcare systems have their work cut out for them. By making small investments in early detection, payers can prevent the considerable costs of treatment down the line. The rise of value-based care has created a unique alignment of incentives that can ease the CKD burden by cutting costs—and saving lives.







